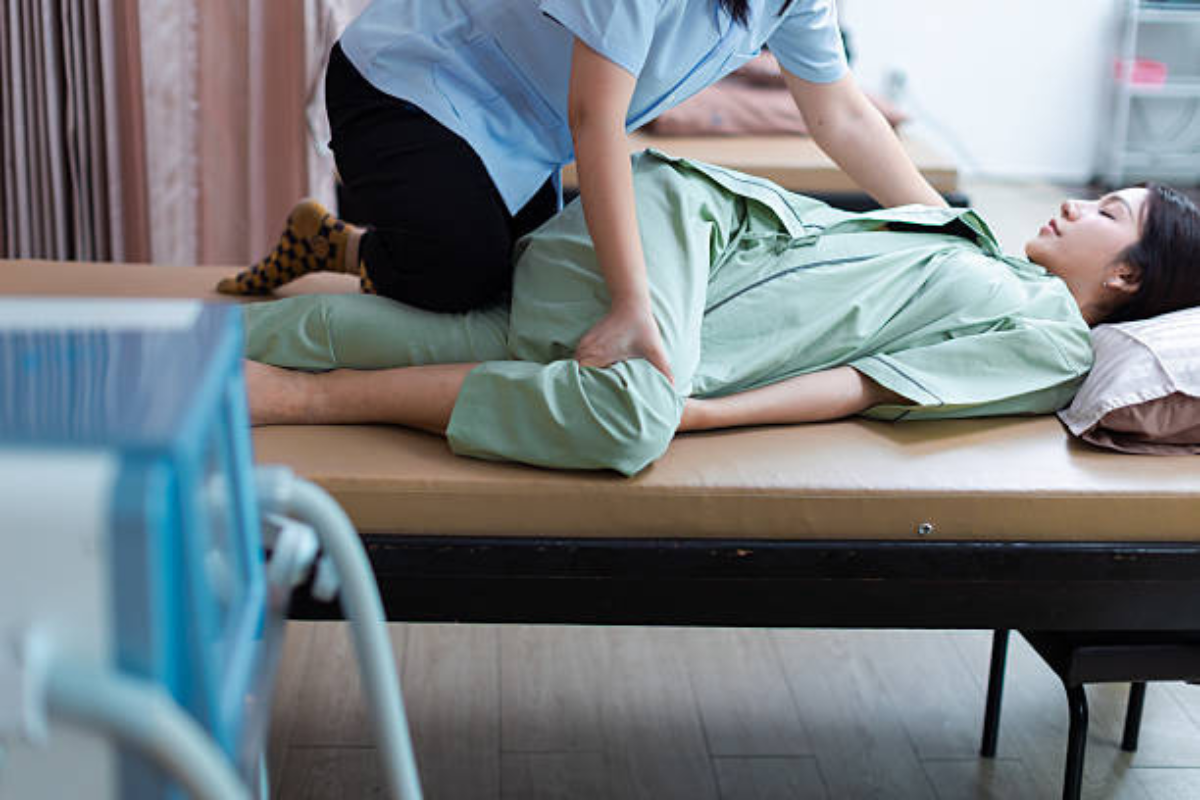
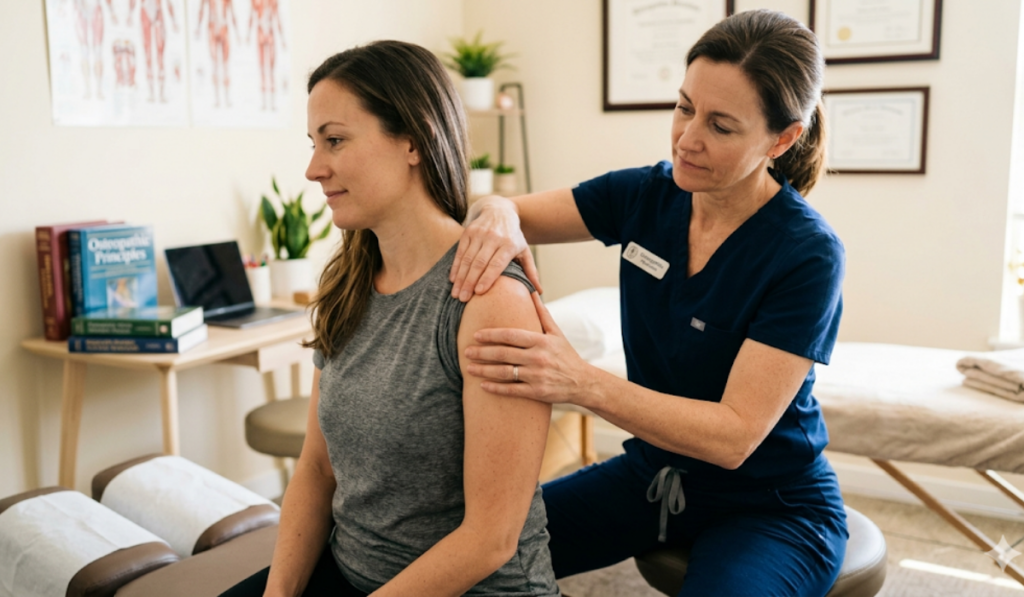
Sciatica can be confusing and frustrating—especially when the pain travels.
One day it’s a deep ache in the low back or buttock. Another day it becomes sharp, burning, or “electric” pain down the leg. Sitting may trigger it. Standing may trigger it. Even sleep can be hard.
TL;DR: Sciatica is nerve-related pain that commonly runs from the low back or buttock down the leg. Many cases improve when you reduce irritation along the nerve pathway—especially when tight hip/glute muscles and trigger points are part of the problem.
Medical disclaimer: This article is for educational purposes and doesn’t replace medical advice or diagnosis. If you have red-flag symptoms (listed below), seek urgent medical care.
What Is Sciatica?
Common Sciatica Symptoms
Sciatica symptoms usually affect one side of the body and may include:
- Pain starting in the low back, hip, or buttock and traveling down the leg
- Burning, shooting, stabbing, or “electric” sensations
- Tingling (“pins and needles”) or numbness
- Weakness or heaviness in the leg (more concerning when progressive)
- Pain that worsens with sitting, bending, or long car rides
If symptoms persist, a clinician can help determine whether your sciatica is primarily muscular, joint-related, or disc-related.
What Causes Sciatica?

Sciatica happens when the nerve (or nerve roots that feed it) gets irritated somewhere along its path. Common causes include:
1) Muscle Tightness and Trigger Points
Tight muscles in the hips and glutes can irritate tissues around the nerve—or create referral patterns that feel like sciatica.
A key muscle is the piriformis, a deep glute muscle close to the sciatic nerve. When it tightens, symptoms can resemble “nerve entrapment” patterns (often discussed as piriformis syndrome).
Other muscles that frequently contribute:
- Gluteus medius/minimus
- Hip flexors
- Hamstrings
- Quadratus lumborum (QL)
- Deep hip rotators
2) Disc Irritation or Bulge
A bulging or herniated disc can press on nerve roots in the low back, creating radiating pain and sensory changes.
3) Spinal Stenosis or Joint Irritation
Narrowing around spinal nerves (stenosis) or irritated facet/SI joints can also refer symptoms into the leg.
4) Prolonged Sitting and Posture Stress
Long periods of sitting can overload hips and low back and increase protective tension, which can aggravate symptoms.
In real life, sciatica is often multifactorial—a mix of posture stress + muscle guarding + joint restriction.
How Medical Massage Can Help Sciatica
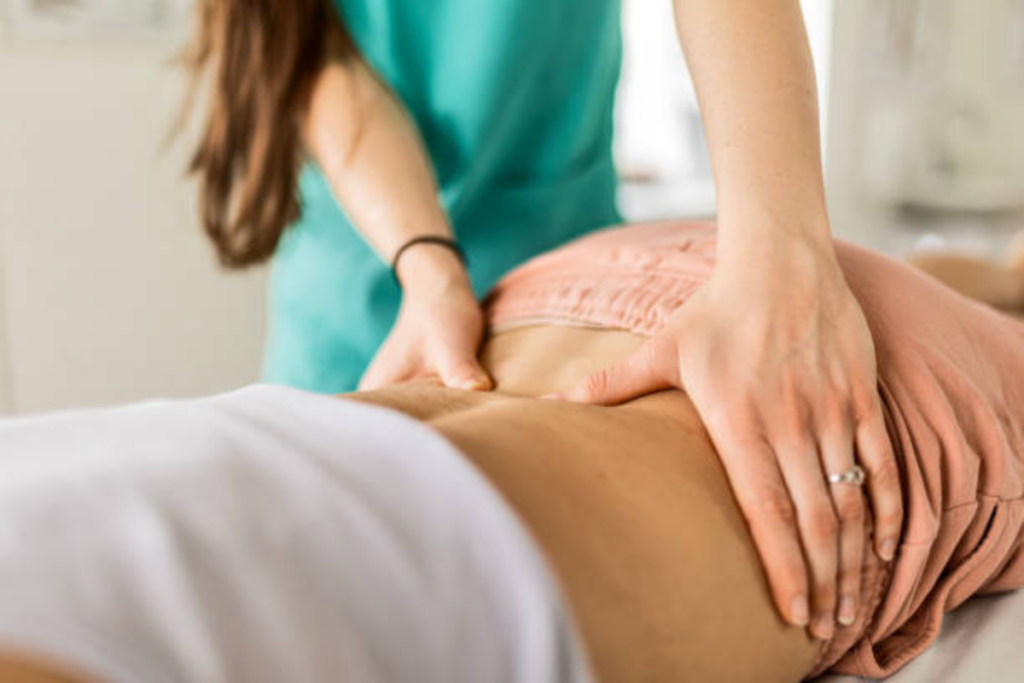
Medical massage (clinical/therapeutic massage) focuses on function and pain reduction—not just relaxation. When sciatica symptoms are influenced by muscular tension and soft-tissue restriction, it can be especially helpful.
1) Reduces Muscle Compression Around the Nerve
Tight hip and glute tissues can reduce comfort and tolerance for sitting/walking. Massage can help those tissues relax and move more freely.
2) Releases Trigger Points That Refer Pain Down the Leg
Trigger points in the glutes and hip rotators can refer pain into the thigh, calf, or foot—sometimes mimicking nerve pain patterns. Targeted work may reduce this referral.
3) Improves Mobility in the Hips and Low Back
Limited hip motion can force the low back to compensate. Massage supports soft-tissue mobility so movement becomes smoother and less painful.
4) Supports Circulation and Recovery
Therapeutic work can reduce protective guarding and support local circulation, helping recovery after flare-ups.
5) Calms an Overprotective Nervous System
Persistent pain can keep your system “on alert.” Gentle-to-moderate clinical massage can help downshift sensitivity (especially when sessions stay within your tolerance).
What a Sciatica-Focused Massage Assessment Looks Like
Medical massage shouldn’t be a one-size-fits-all routine. A skilled therapist typically starts with a brief intake to understand what aggravates or eases symptoms, then tailors treatment.
Common screening questions and observations may include:
- Symptom behavior: Is it worse sitting, standing, walking, or bending?
- Pain path: Does it start in the low back/buttock and travel down the leg?
- Movement tolerance: Hip rotation, hamstring tension, low-back stiffness
- Tenderness patterns: Glute/piriformis sensitivity and referral patterns
- Irritability level: How easily symptoms flare with pressure or stretching?
This helps the therapist choose the right techniques and pressure—because overly aggressive work can flare symptoms in some people.
When Massage Helps Most vs. When to See a Doctor First
Massage tends to help most when:
- Symptoms are strongly linked to tight hips/glutes, trigger points, and limited mobility
- Sitting/posture patterns clearly flare symptoms, and soft-tissue tension is prominent
- You have recurring flare-ups tied to workload, stress, or prolonged sitting
Seek medical evaluation urgently (instead of massage) if you have:
- Bowel or bladder changes (especially new loss of control)
- Progressive leg weakness
- Severe or rapidly worsening numbness
- Symptoms after major trauma, or concerning systemic symptoms (like fever)
These can indicate conditions that require prompt evaluation.
What Type of Massage Is Best for Sciatica?

The “best” approach depends on irritability and what’s contributing to your symptoms. Common clinical techniques include:
- Myofascial release
- Deep tissue (as tolerated)
- Trigger point therapy (often glutes, piriformis, hamstrings)
- Neuromuscular techniques
A skilled therapist will adjust pressure based on sensitivity—because too much intensity too soon can flare symptoms.
What Areas Are Typically Treated?
- Lower back and paraspinals
- Glutes (including deep glute work)
- Piriformis and hip rotators
- Hamstrings
- Hip flexors (in some cases)
- Calves/feet if symptoms travel that far
What to Expect After a Session
- Less tightness in the glutes/hips
- Improved walking comfort
- Reduced intensity or frequency of leg pain
- Better ability to sit or stand
- Temporary soreness (similar to post-workout fatigue)
If symptoms are highly sensitive, improvement may happen gradually over multiple sessions.
How Many Sessions Are Usually Needed?

It depends on the cause, severity, and duration:
- Recent flare-ups: sometimes 1–3 sessions can create meaningful change
- Chronic sciatica: often needs a short plan (commonly 4–8 sessions)
- Maintenance/prevention: periodic sessions may help prevent relapse if posture or activity patterns keep re-triggering tension
Massage is often most effective when paired with simple movement changes—like walking, posture breaks, and gentle stretching.
Self-Care Tips That Often Help Between Sessions
Keep this simple and consistent:
- Take posture breaks: stand/walk 2–5 minutes every 30–45 minutes
- Walk daily: short walks can reduce stiffness and nerve sensitivity
- Gentle hip stretching: avoid aggressive stretching into sharp pain
- Heat for muscle tightness: 10–15 minutes can help relax tissues
- Sleep support: pillow between knees (side sleeping) or under knees (back sleeping)
If pain worsens with a specific stretch or position, stop and reassess.
When to Get Medical Attention Instead of Massage
- Loss of bowel or bladder control
- Progressive leg weakness
- Severe or rapidly worsening numbness
- Fever, unexplained weight loss, or pain after major trauma
- Pain that is constant, extreme, and not improving at all
FAQs

1) Can medical massage help sciatica?
Yes. Medical massage may reduce sciatica symptoms when tight muscles and trigger points irritate the sciatic nerve. It can ease tension, improve movement, and reduce pain.
2) What type of massage is best for sciatica?
Clinical techniques like myofascial release, deep tissue (as tolerated), and trigger point therapy are commonly used—especially for the glutes, piriformis, and hamstrings.
3) How many sessions does it take to relieve sciatica with massage?
Some people feel changes within 1–3 sessions. More persistent sciatica may require a short plan (often 4–8 sessions), depending on the cause and how long symptoms have lasted.
4) Where should massage focus for sciatica?
Often the low back, glutes, piriformis, hips, hamstrings, and sometimes calves—based on where the nerve irritation begins and how pain travels.
5) When should you avoid massage for sciatica?
Avoid massage and seek urgent medical care if you have worsening weakness, severe numbness, loss of bowel/bladder control, fever, or major trauma.
Conclusion
Sciatica isn’t always a “back problem.” Often, it’s a nerve irritation pattern made worse by tight hips, deep glute tension, and trigger points.
When we reduce that tension and improve movement, symptoms often ease—and flare-ups become less frequent.