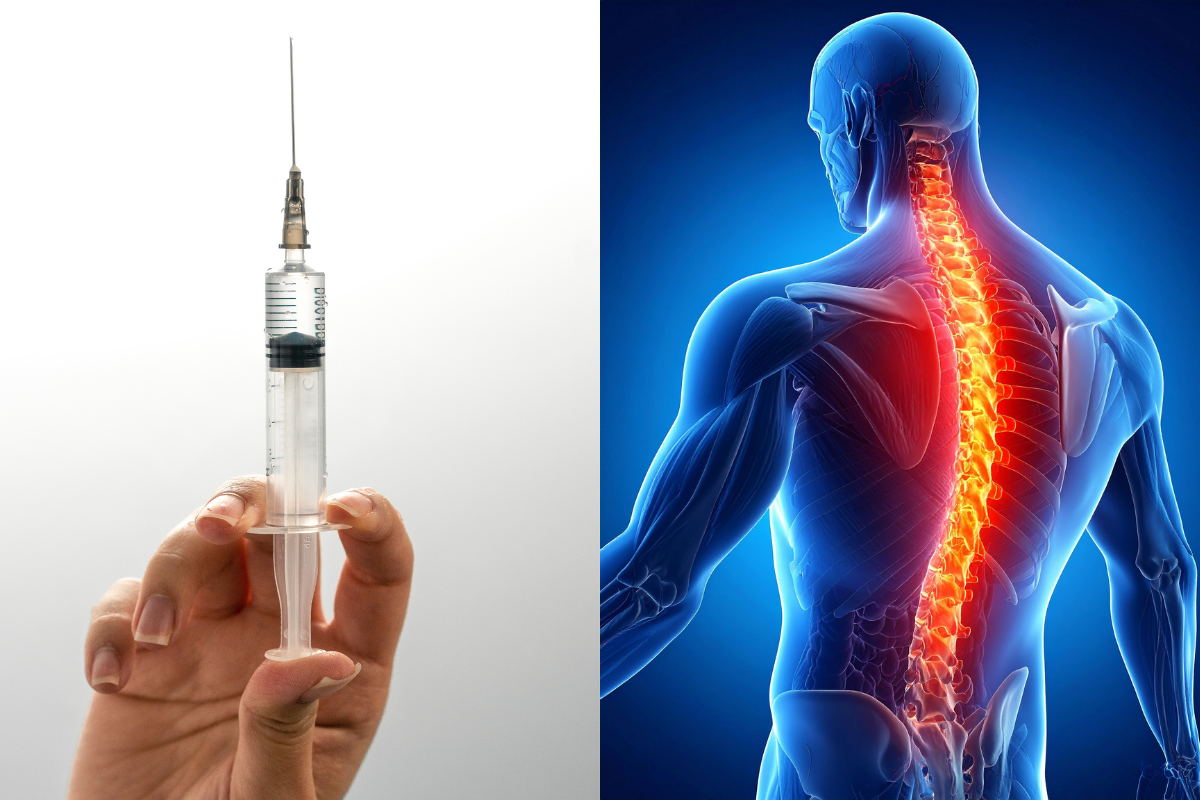
Can trigger point injections help sciatica-like pain from piriformis syndrome?
Yes—trigger point injections for piriformis syndrome may help some people with sciatica-like symptoms when the pain source is muscular rather than spinal. By calming piriformis muscle spasm and reducing local irritation near the sciatic nerve, trigger point injections can support improved movement and rehabilitation—especially when combined with guided therapy and root-cause care.
Before we begin
What “sciatica-like pain” really means
Sciatica is not a diagnosis—it’s a symptom pattern. Medically, sciatica refers to pain that follows the course of the sciatic nerve, often with numbness, tingling, or weakness.
Many people hear “sciatica” and assume it automatically means a bulging disc or pinched nerve in the spine. But in real-world practice, leg pain can come from several sources, including:
- Lumbar disc irritation or herniation
- Spinal stenosis
- Sacroiliac joint dysfunction
- Hip joint involvement
- Myofascial trigger points (especially in the glutes)
- Piriformis syndrome / deep gluteal syndrome
Why it matters: Treatments that help disc-related sciatica may not help piriformis-related pain, and vice versa.
What is piriformis syndrome?

Piriformis syndrome occurs when the piriformis muscle—a small but powerful deep hip rotator—becomes tight, irritated, or overworked and compresses or irritates the sciatic nerve in the buttock region.
Common symptoms of piriformis syndrome
People often describe:
- Deep, aching pain in the buttock (sometimes “like sitting on a golf ball”)
- Pain that worsens with sitting, driving, or prolonged hip flexion
- Tenderness in the glute region
- Sciatica-like pain traveling down the back of the thigh
- Occasional tingling or numbness, usually less intense than spine-based sciatica
Patterns we commonly see clinically
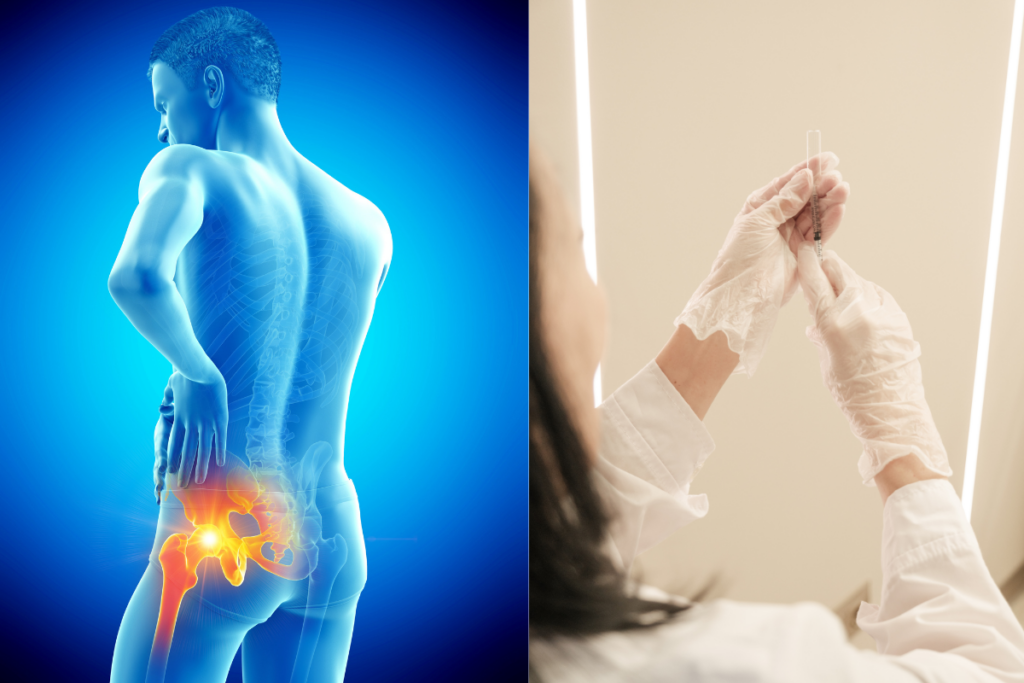
In integrative and functional musculoskeletal care, piriformis syndrome often shows up alongside:
- Prolonged sitting and poor hip mobility
- Pelvic instability or “glute weakness”
- Overuse from walking/running/hills
- Postural strain (especially from desk work)
- Compensation patterns after low back pain episodes
Piriformis pain is rarely “random.” It usually has mechanical and neuromuscular drivers that can be identified and addressed.
How piriformis syndrome causes sciatica-like symptoms
The sciatic nerve travels through the pelvis and passes close to the piriformis muscle. When the piriformis becomes hypertonic (excessively tight) or develops trigger points, it can:
- Increase localized pressure near the nerve
- Create inflammation-like irritation around sensitive tissues
- Reduce normal blood flow and glide in the region
- Refer pain downward in a pattern that mimics nerve pain
In some anatomical variations, the sciatic nerve pathway can make irritation more likely (though this isn’t required for symptoms to occur).
Piriformis syndrome vs true lumbar sciatica: how they are different
| Feature | True Sciatica (Spinal) | Piriformis Syndrome (Muscular) |
|---|---|---|
| Primary source | Nerve root irritation in the low back | Sciatic nerve irritation in the buttock |
| Common starting point | Lower back pain often present | Deep buttock pain often dominant |
| Pain triggers | Coughing, bending, spinal motion may worsen | Sitting, driving, hip rotation often worsen |
| Radiation pattern | Often down the leg to the foot | Often buttock → thigh (can go lower in some cases) |
| Key focus of treatment | Spine and nerve root mechanics | Hip and deep gluteal muscle function |
Clinical takeaway:
Pain that behaves like sciatica doesn’t always originate in the spine. A careful exam can be the difference between guessing and targeted care.
What are trigger point injections and how do they work?
Trigger point injections (TPIs) are a procedure used to treat painful knots (trigger points) within muscle tissue that contribute to:
- Local pain
- Referred pain patterns
- Movement restriction
- Protective muscle guarding
Trigger points are commonly encountered and can contribute to myofascial pain syndromes.
What’s injected?
- A small amount of local anesthetic (commonly used)
- Saline solution
- Occasionally other options based on provider preference and safety considerations
How trigger point injections may help piriformis syndrome
- Reducing piriformis muscle hypertonicity
- Decreasing localized nerve irritation
- Improving circulation and oxygen delivery
- Restoring more normal movement patterns
- Making stretching and strengthening more tolerable afterward
Benefits and realistic expectations
Potential benefits
- Reduced buttock tightness and spasm
- Less radiating leg discomfort
- Easier walking and improved hip motion
- Better tolerance to rehab and strengthening
- Improved sleep and sitting tolerance
What TPIs can’t do
- TPIs do not treat disc herniations
- TPIs do not correct spinal stenosis
- TPIs do not replace strength, stability, and movement retraining
- TPIs are not a cure-all for every form of sciatica
If your symptoms are driven by lumbar nerve root compression, a different treatment plan may be more appropriate.
How long does relief typically last?
This varies widely. In clinical practice, response depends on:
- How long the muscle has been dysfunctional
- Whether biomechanics are corrected after the injection
- Activity level, sitting demands, and hip mobility
- Whether other contributors exist (SI joint, lumbar spine, glute med weakness, etc.)
Some people feel improvement in days; others notice gradual change over 1–2 weeks as movement patterns normalize.
A helpful way to think about it:
The injection may create a “therapeutic window.” What you do with that window—mobility, neuromuscular retraining, strength, posture, gait—often determines the long-term outcome.
Are trigger point injections safe?
In the hands of trained clinicians, trigger point injections are generally considered a low-risk procedure, but no medical procedure is risk-free.
Common side effects
- Temporary soreness at the injection site
- Mild bruising
- Short-term flare of symptoms
- Temporary numbness (if anesthetic is used)
Less common risks (but important to know)
- Bleeding or infection
- Nerve irritation
- Vasovagal response (lightheadedness/fainting)
- Allergic reaction (rare)
Who may not be a good candidate?
Trigger point injections may not be appropriate if you have:
- Active infection or fever
- Uncontrolled bleeding disorders or certain anticoagulant situations (provider-dependent)
- Allergy to injectate ingredients
- Unexplained progressive neurological weakness
- Red-flag symptoms suggesting urgent spinal or systemic causes
When to seek urgent medical evaluation
Seek urgent care if you have:
- New bowel or bladder dysfunction
- Severe or progressive leg weakness
- Saddle numbness
- Significant unexplained fever with back pain
Notes: Sciatica can be associated with serious symptoms in some cases and may require urgent evaluation, especially when weakness or bowel/bladder changes occur.
Circle Wellness’s integrative approach to piriformis-related pain
At Circle Wellness, we treat sciatica-like pain with a root-cause lens. That means we don’t assume the spine is the problem—or that the piriformis is the problem—until we evaluate the full picture.
Step 1: We differentiate the “why”
We start with a careful assessment to distinguish whether symptoms are more consistent with:
- Lumbar radiculopathy (true nerve root sciatica)
- Piriformis syndrome or deep gluteal pain
- SI joint dysfunction
- Hip mobility restrictions or instability patterns
- Myofascial trigger point referral patterns
Step 2: We address the driver, not just the symptom
When piriformis involvement is likely, treatment may include:
- Myofascial trigger point therapy piriformis (hands-on + neuromuscular techniques)
- Targeted mobility work (hip rotation, posterior chain)
- Core + pelvic stabilization
- Gait and posture correction
- Movement retraining for sitting-heavy lifestyles
Step 3: We use injections strategically
If conservative care is limited by severe muscle guarding or pain, trigger point injections for piriformis syndrome may be used to:
- Decrease protective tension
- Reduce pain amplification
- Improve tolerance to therapy
- Support functional progress
This is integrative sciatica treatment the way it should be—carefully individualized and tied to a plan.
Practical next steps you can take today
If you suspect piriformis involvement, consider these steps:
1) Track your triggers
- Does sitting worsen symptoms?
- Do hills/stairs flare it?
- Is it better after walking?
- Does stretching help briefly, then rebound?
2) Focus on movement breaks
Every 30–45 minutes:
- Stand up
- Walk for 1–2 minutes
- Do gentle hip mobility
3) Don’t stretch aggressively into nerve pain
Some “piriformis stretches” can irritate the nerve if done too forcefully. A clinician can help tailor this safely.
4) Get assessed before assuming it’s “just sciatica”
Sciatica-like pain deserves a real evaluation—not a label.
FAQs

1) What is the fastest way to tell if it’s piriformis syndrome or sciatica?
A detailed exam is often more helpful than guessing. Piriformis-related pain tends to be more buttock-centered and aggravated by sitting or hip mechanics, while true sciatica often links to spinal nerve root irritation.
2) Do trigger point injections treat the sciatic nerve directly?
No. Trigger point injections target the muscle tissue, not the nerve itself. The goal is to reduce muscle tension and local irritation that may be contributing to sciatica-like symptoms.
3) Are trigger point injections painful?
Most patients describe them as brief pressure or a quick pinch, followed by temporary soreness—similar to a deep workout sensation. Comfort strategies can be used based on sensitivity.
4) How many injections will I need?
It depends on the driver of dysfunction and how well the body responds to combined care. Some people improve after one session; others benefit from a short series integrated with rehab and movement correction.
5) Can piriformis injections replace physical therapy?
Usually no. In many cases, the best outcomes occur when injections are used to support active recovery, not replace it.
6) Can piriformis syndrome come from sitting too much?
Yes. Prolonged sitting can overload deep hip rotators, reduce glute activation, and contribute to tension patterns that aggravate piriformis-related pain—especially when combined with weak pelvic stabilizers.
7) What if my MRI shows a disc bulge?
Disc changes are common and don’t always explain symptoms. A clinical correlation is essential. Some people have disc findings but primarily muscular drivers; others truly have lumbar nerve irritation. The exam helps clarify the most likely pain generator.
Key takeaways
- Sciatica is a symptom pattern, not a diagnosis.
- Piriformis syndrome can mimic sciatica, because the piriformis can irritate the sciatic nerve in the buttock.
- Trigger point injections for piriformis syndrome may help reduce muscle spasm and improve function when used appropriately.
- TPIs don’t treat every cause of sciatica-like pain, especially spinal nerve root compression.
- The most effective care plans are usually integrative: assessment → targeted therapy → injections only when helpful → rehab for lasting results.
Medical Disclaimer
This content is for educational purposes only and is not intended to diagnose, treat, cure, or prevent any medical condition. Always consult a qualified healthcare provider for personalized medical advice.