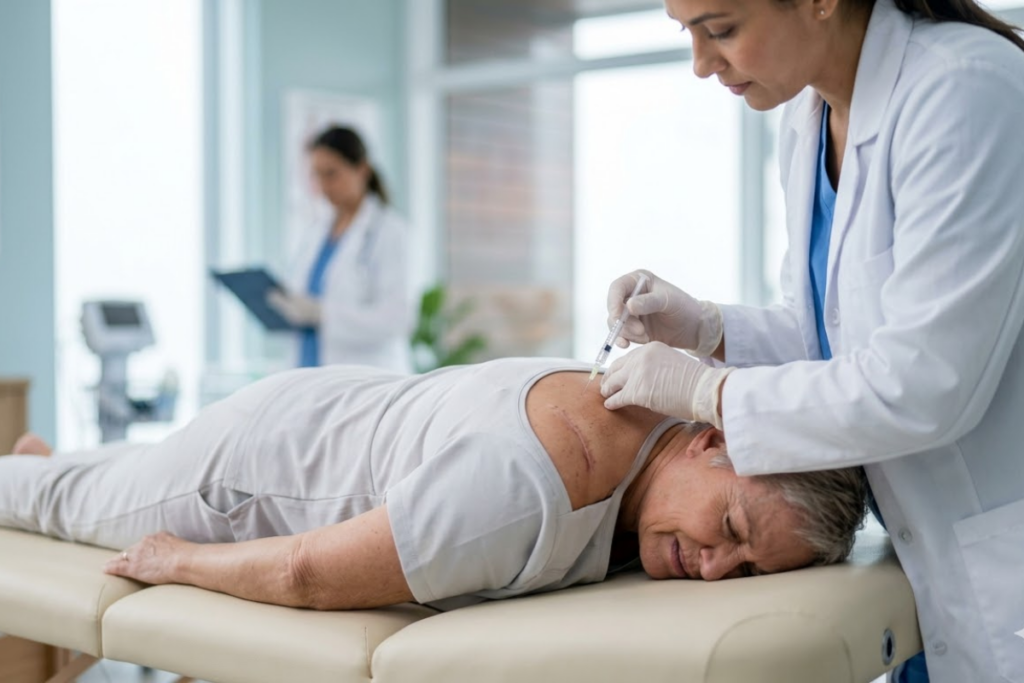
Headaches can be exhausting—not just physically, but emotionally. When pain becomes frequent, unpredictable, or hard to “treat your way out of,” it can start to affect sleep, productivity, mood, and your sense of control in daily life.
One option that may help certain headache patterns—particularly those tied to myofascial tension—is trigger point injections (TPI). These injections are not a cure for migraines, and they aren’t the right fit for everyone. But for the right patient, used thoughtfully and as part of a broader plan, they can reduce local muscle irritability and help calm referred pain patterns.
This article is designed to explain trigger point injections for headaches in a medically responsible, patient-first way—so you can make informed decisions with your healthcare provider.
Can trigger point injections help tension headaches and migraines?
Tension Headaches vs Migraines: What’s the Difference?
Although both can be disabling, tension headaches and migraines are not the same condition—and they often need different strategies.
Tension-Type Headaches
Tension headaches are often associated with muscle tightness and mechanical strain. Many people describe:
- A dull, aching pressure (often “band-like”)
- Tightness around the forehead, temples, or back of the head
- Neck and shoulder tension
Pain that builds gradually through the day
Some patients can still function, but the discomfort is persistent and draining.
Migraines
Migraine is a neurological disorder involving abnormal signaling in the nervous system and brain blood vessels. It’s commonly associated with:
- Moderate to severe head pain (often throbbing or pulsing)
- Nausea and/or vomiting
- Sensitivity to light and sound
Possible aura symptoms (visual or sensory changes)
NIH sources describe migraine as a condition involving abnormal activity among nerve signals, chemical signals, and blood vessels in the brain. (NINDS)
Why the Overlap Matters
Here’s the important clinical nuance: muscle trigger points do not “cause” migraine in the way genetics and neurology do—but muscle tension can still contribute to attacks, amplify pain intensity, and prolong recovery in some patients.
In real-world clinical care, we often see migraine patients with a major musculoskeletal component:
- Forward-head posture or desk strain
- Tight upper trapezius and suboccipital muscles
- Jaw clenching (bruxism) and TMJ overload
- Shoulder/upper-back overuse
When these patterns are present, treating trigger points may help reduce one layer of the overall headache burden.
What Are Trigger Points?

A trigger point is a hyperirritable spot in a taut band of muscle that can cause:
- Local tenderness
- Tightness and reduced mobility
- Referred pain (pain felt in a different region)
In other words: you press one spot in the neck or shoulder, and the person feels pain in the head, temple, behind the eye, or jaw.
Trigger points often develop when muscles are under chronic stress, including:
- Prolonged posture strain (screens, driving, studying)
- Repetitive overload (lifting, carrying, overhead work)
- Sleep position issues
- Dehydration or poor recovery capacity
- Emotional stress and nervous system sensitization
- Old injuries (whiplash, concussion history, shoulder injuries)
Over time, the muscle becomes “stuck” in a guarded state—constantly signaling irritation to surrounding tissues and the nervous system.
How Muscle Trigger Points Can Drive Headache Patterns
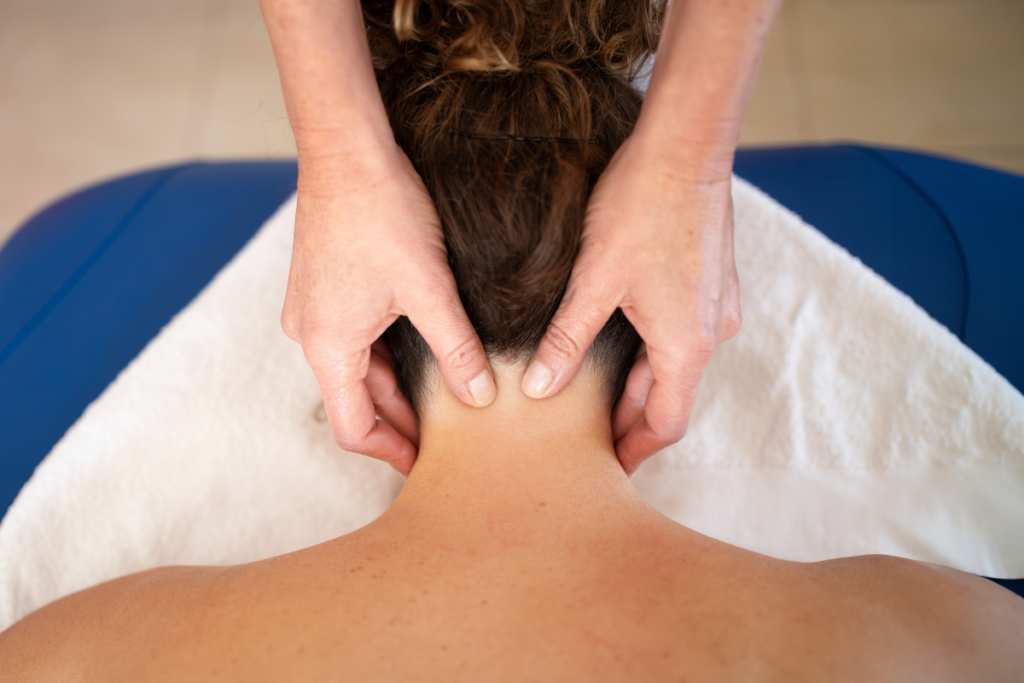
Many headache patterns have a myofascial component, meaning the pain is influenced by muscles and fascia (connective tissue). This is especially relevant for:
1) Cervicogenic and “Tension-Dominant” Headaches
Neck and upper-back muscles can refer pain upward to the base of the skull and temples.
2) Migraine With Neck Pain
A large number of migraine patients report significant neck pain before or during attacks. Sometimes this is part of the migraine itself; other times it’s a parallel driver that increases vulnerability.
3) Headaches Tied to Jaw Clenching
Jaw tension can irritate the temporalis and masseter muscles, contributing to temple pain and facial discomfort.
In clinical practice, a careful exam often shows that treating trigger points can reduce pain intensity and improve range of motion—even when a neurological migraine diagnosis remains.
What Are Trigger Point Injections?
- A small amount of local anesthetic (commonly used)
- Saline (in some approaches)
- Or “dry needling” technique (needle stimulation without medication)
How Do Trigger Point Injections Work?
Trigger point injections may help by addressing three common issues seen with myofascial pain:
1) Reducing Local Muscle Hyperirritability
Trigger points are often electrically and chemically “overactive.” Needling the area can help interrupt that cycle.
2) Improving Local Circulation
A tight muscle band can reduce normal blood flow and oxygen delivery. Releasing it may support healthier tissue recovery.
3) Decreasing Referred Pain Patterns
Some trigger points refer pain into the head and face. When the trigger point calms down, the referred pain often reduces as well.
Many patients describe improved mobility in the neck and shoulders—along with less “pulling,” pressure, or heaviness in the head.
Common Trigger Point Locations Linked to Headache Pain
Below are muscle regions Circle Wellness clinicians frequently evaluate when headaches are part of the complaint.
Neck and Upper Trapezius
These muscles commonly tighten under:
- Screen posture
- Stress and shallow breathing
- Shoulder elevation and guarding
Referral pattern: Side of the head, temple, behind the eye
Suboccipital Muscles (Base of the Skull)
These small muscles can become overactive when the head sits forward on the neck.
Referral pattern: Back of the head, “ram’s horn” headache pattern, deep ache behind the eyes
Jaw and Temporalis Muscles
Commonly involved with:
- Clenching and grinding
- TMJ overload
- Chewing asymmetry
Referral pattern: Temple pain, facial tightness, tooth-like pain without dental cause
Shoulder and Upper Back Muscles
Often involved with:
- Carrying loads
- Reaching/overhead activity
- Breathing pattern dysfunction
Referral pattern: Neck tension, head heaviness, pressure behind the head
Benefits and Realistic Expectations

Trigger point injections can be helpful, but only when used appropriately.
What TPIs may help with
- Less muscle “pulling” and neck tightness
- Reduced referred pain into the head and face
- Fewer tension-dominant headache days
- Improved neck range of motion
- Better tolerance for posture work, PT, or rehab
What TPIs cannot promise
- TPIs do not cure migraine
- TPIs may not help headaches driven by primarily neurological, vascular, hormonal, or medication-related factors
- Some patients feel only mild or temporary benefit
How Long Does Relief Typically Last?
Relief varies based on:
- How long trigger points have been active
- Stress load and sleep quality
- Posture, ergonomics, and muscle conditioning
- Whether underlying drivers are addressed
Some people notice improvement within 24–72 hours. Others need a series of treatments alongside therapy and movement retraining. Relief may last days to weeks, and for some patients, longer—especially when combined with corrective care.
A key clinical goal is not just short-term relief, but improved resilience so the trigger points don’t immediately reactivate.
Are Trigger Point Injections Safe?
When performed by trained clinicians, TPIs are generally considered a low-risk procedure. However, “low risk” doesn’t mean “no risk.”
Common side effects
- Temporary soreness or bruising at the injection site
- Mild swelling
- Short-lived increase in pain (“post-injection flare”)
- Fatigue or lightheadedness
Less common risks (but important)
- Infection (rare)
- Bleeding or hematoma risk (higher in certain patients)
- Nerve irritation
- Allergic reaction (depending on substances used)
Special caution areas
Injections around the upper back/neck require skilled technique due to nearby structures. This is one reason TPIs should be performed in a medically supervised setting.
Who May Not Be a Good Candidate?
- A bleeding disorder or are on certain blood thinners (case-by-case)
- Active infection or skin irritation at the injection site
- Certain medication allergies (if anesthetic is used)
- Severe needle phobia without adequate support
- Unclear headache red flags that need urgent evaluation first
Circle Wellness’s Integrative Approach to Headache Treatment

At Circle Wellness, we view headaches through a root-cause lens. That means we don’t assume one “magic intervention” fits everyone, even when trigger points are clearly involved.
In our clinical experience, headache patterns often reflect a stack of contributors, such as:
- Musculoskeletal strain (neck, jaw, shoulders)
- Nervous system sensitization and stress physiology
- Sleep disruption and recovery deficits
- Posture and breathing mechanics
- Prior injuries (whiplash, concussion, falls)
- Inflammatory drivers that increase pain sensitivity
What makes an integrative plan different?
- Myofascial trigger point therapy (manual + injection options)
- Neuromuscular re-education and posture retraining
- Gentle mobility and stabilization programs
- Breathwork strategies for downshifting muscle guarding
- Lifestyle and recovery support (sleep, hydration, nutrition)
- Coordinated care with headache specialists when needed
Practical Next Steps If You Suspect Trigger Points Are Involved
If your headaches seem connected to muscle tension, here are patient-safe steps that may help guide your next visit:
Track patterns for 1–2 weeks
Note:
- Where pain begins (neck, temple, behind the eye, jaw)
- Time of day patterns (afternoon posture fatigue is common)
- Triggers (stress, sleep loss, workouts, screens)
- Associated symptoms (nausea, light sensitivity, aura)
Pay attention to these clues
Trigger points may be involved when:
- Neck/shoulder tightness is present most days
- Head pain worsens with posture or stress
- Massage temporarily helps—but pain returns quickly
- You feel “knots” that reproduce head pain when pressed
Ask for an exam—not just a prescription
A high-quality headache evaluation includes:
- Neck mobility and posture assessment
- Palpation of key muscle groups
- Screening for jaw involvement
- Discussion of migraine vs tension features
Tension Headache vs Migraine vs Myofascial Pain Overlay
| Feature | Tension-Type Headache | Migraine | Myofascial Trigger Point Overlay |
|---|---|---|---|
| Pain quality | Pressure/tightness | Throbbing/pulsing | Deep ache + referred pain |
| Common areas | Forehead, temples, band-like | One side, behind eye | Neck → head/face referral |
| Symptoms | Mild nausea sometimes | Nausea, light/sound sensitivity | Stiffness, tender knots |
| Key drivers | Stress, posture, muscle tension | Neurological sensitization | Muscle overload + guarding |
| TPI role | Often helpful if trigger points present | May help muscle-driven component | Directly targeted |
FAQs

1) What is the fastest way to tell if it’s piriformis syndrome or sciatica?
They may help some migraine patients when muscular trigger points are contributing to neck, jaw, or shoulder tension, but they do not cure migraine. NIH sources describe migraine as a neurological condition involving abnormal signaling and blood vessel activation in the brain.g
2) What muscles are most involved in tension headache trigger points?
Common muscle groups include the upper trapezius, suboccipitals (base of the skull), sternocleidomastoid, temporalis, and jaw muscles—especially in people with posture strain or clenching.
3) How many trigger point injections will I need?
It depends on chronicity, trigger point density, and underlying drivers. Some patients benefit from 1–3 sessions, while others need a longer plan paired with rehab and nervous system support.
4) Do trigger point injections hurt?
Most people describe brief discomfort and pressure rather than severe pain. Some soreness afterward is common for 24–48 hours, similar to how muscles can feel after deep bodywork.
5) How long does relief last?
Relief varies. Some feel improvement for days; others for weeks. Long-term results are more likely when TPIs are paired with posture correction, mobility work, and stress-load reduction.
6) Are trigger point injections safe in the neck?
They can be safe when performed by a trained clinician using appropriate technique. The neck and upper back contain sensitive structures, which is why medical training and careful assessment matter.
7) What else should be done alongside TPIs?
Many patients do best with combination care, such as manual therapy, strength/stability work, ergonomic changes, sleep optimization, and migraine-specific coordination when appropriate.
Key Takeaways
- Trigger points are hyperirritable muscle knots that can refer pain into the head, face, and jaw.
- Tension headaches are often muscle-driven, while migraines are neurological, though muscle tension can worsen migraine burden.
- Trigger point injections for headaches may help reduce muscle hyperirritability and referred pain patterns.
- TPIs are best viewed as one tool in a comprehensive plan—not a cure.
- Safer, longer-lasting outcomes often come from combining injections with rehab, posture support, and nervous system regulation.
Medical Disclaimer
This content is for educational purposes only and is not intended to diagnose, treat, cure, or prevent any medical condition. Always consult a qualified healthcare provider for personalized medical advice.